Ema appliance4/2/2023   
The high proportion of posterior openbites described, and magnitude of overbite/overjet changes are speculated to influence functional occlusion, aesthetics and speech but this is poorly understood and warrants further research. Although this study highlights dental occlusal changes that are progressive with MAS use, the impact of a patient's perception of bite changes on long term adherence was not specifically addressed. The motivation to use a MAS represents a delicate balance between a patient's perception of therapeutic efficacy, comfort and side effects. Like CPAP therapy, MAS effectiveness is impacted by adherence. 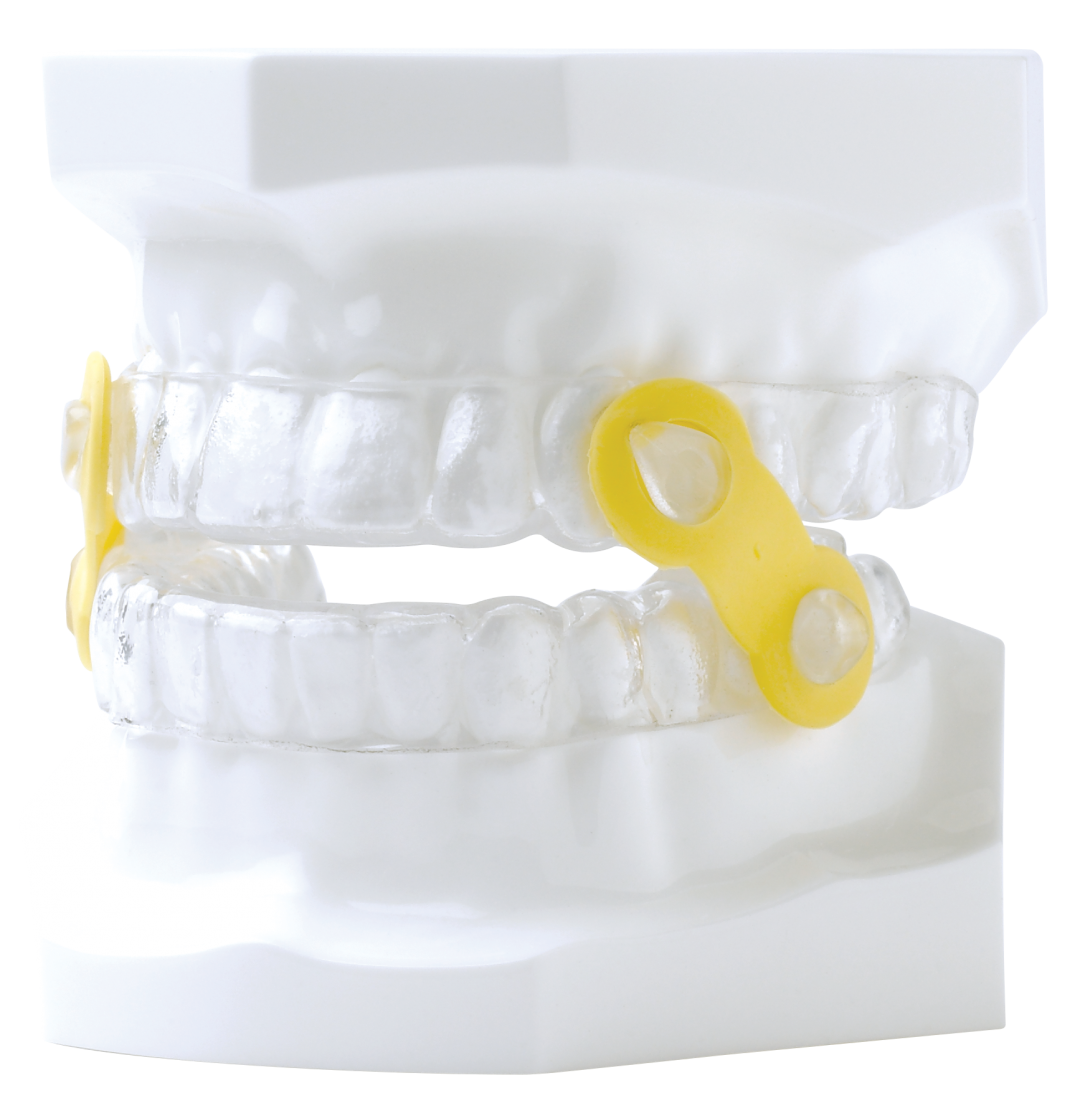
Progressive changes in dental occlusion were observed with overbite and mandibular intermolar distance decreasing less with time, while overjet, mandibular intercanine distance and lower arch crowding all decreasing at a constant rate. 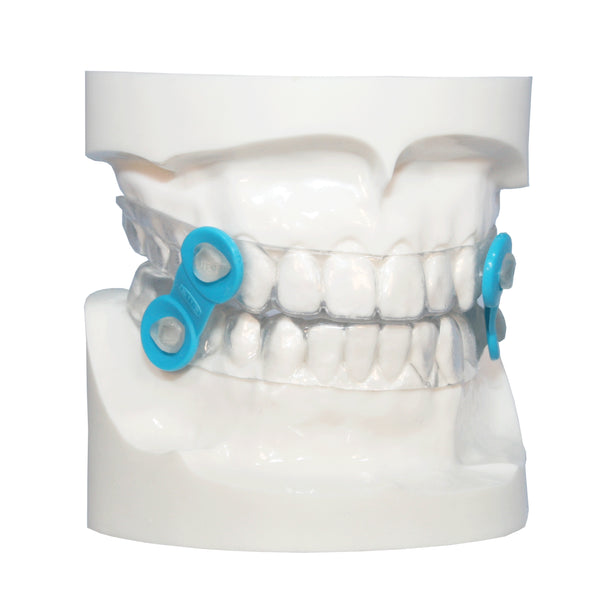
However, in contrast to previous studies, this study highlights that discernible changes in dental side effects do not plateau or reach a discernible end-point but are ongoing with MAS use. 1, 2 The magnitude of overbite (2.3 mm) and overjet (1.9 mm) changes described in this study associated with over a decade of MAS use is greater than previous long term (> 5 years) studies. This study builds on previous work by these authors and others. Moreover, 62% (48/77) of the group also developed an anterior crossbite of at least one tooth with an average of 4 teeth being observed. Half of the patients developed a posterior openbite, defined as a loss of occlusal contact on at least 2 posterior teeth. Interestingly, significant increases in mandibular intercanine (0.7 ± 1.5 mm) and inter-molar widths (1.1 ± 1.4 mm) were found. 77 patients (62 males, mean BMI 29 kg/m 2) including snorers and patients with a broad spectrum of OSA severity were evaluated and found to have significant decreases in overbite (2.3 ± 1.6 mm), overjet (1.9 ± 1.9 mm) and mandibular crowding (1.3 ± 1.8 mm). This landmark longitudinal study, representing the longest follow-up published to date, documented clinically significant changes in occlusion that were progressive over an average of 11 years of MAS use, based on dental study cast analysis. Hence, the paper by Pliska and colleagues 3 in this issue of JCSM is a welcome addition to the literature. 1, 2 The details surrounding the appearance and time course of these changes have been poorly understood. While this augers well for enhancing treatment adherence and treatment outcomes, some unease exists among clinicians and patients about long term side effects.Ī number of studies have demonstrated the appearance of minor, usually subclinical, changes in the dentition over time. This clinical shift toward increasing usage of MAS is underpinned by a growing evidence base that has identified good treatment efficacy for patients across the spectrum of mild to severe OSA and higher patient preference for this form of treatment. Mandibular advancement splints (MAS) are the most common form of oral appliance used in clinical practice and are currently indicated for treatment of mild to moderate OSA patients and severe OSA patients who are intolerant or refuse CPAP therapy. Oral appliance therapy is increasingly recognized as a viable treatment alternative for OSA. Whereas continuous positive airway pressure (CPAP) was more or less the sole effective treatment for many years, the landscape is changing with a growing number of treatment alternatives of varying efficacy, and a move toward personalized care. The treatment of obstructive sleep apnea (OSA) has been undergoing a steady shift over the last decade. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
